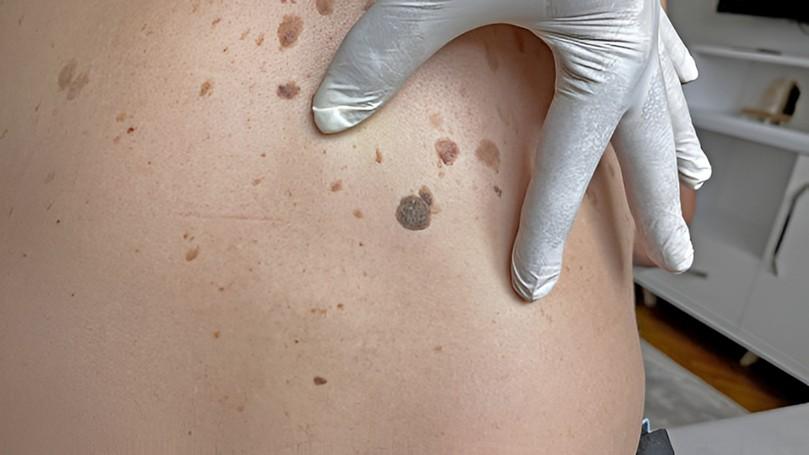
Key Takeaways
- Australia has the highest melanoma incidence rate in the world. Queensland carries the highest risk of any state.
- Approximately 17,443 new melanoma cases are estimated for Australia in 2025, with around 1,455 expected deaths.
- Skin cancer can develop on areas with no sun exposure, including feet, palms, nails, and mucous membranes.
- The ABCDE criteria help identify suspicious lesions, but dangerous cancers can appear without obvious pigmentation.
- Early detection dramatically improves survival outcomes. Melanoma caught early is close to 100 percent curable.
Why Skin Cancer Is So Easily Missed in Australia
Most Australians are aware that skin cancer exists and that sun protection matters. Fewer are aware that skin cancer can look nothing like what they expect, that it can appear in places they never think to check, or that several of the most dangerous forms develop with no symptoms at all until they are advanced.
According to Cancer Australia, melanoma is the third most commonly diagnosed cancer in Australia and it is estimated to cause around 1,455 deaths in 2025. Queensland has consistently recorded Australia’s highest melanoma incidence rate, at approximately 64 cases per 100,000 people compared to a national average of around 48. Living on the Gold Coast puts you directly in one of the highest risk regions in the country.
The problem is not only UV exposure. It is also recognition. People delay seeking medical attention because a spot does not look the way they expect skin cancer to look. The following warning signs are those most frequently overlooked.
Sign 1: A Spot That Does Not Look Like a Mole
Many Australians associate skin cancer with a dark, irregular mole. This is an understandable but dangerous oversimplification. The three most common forms of skin cancer look very different from each other, and two of them are rarely darkly pigmented at all.
Basal cell carcinoma (BCC) is the most common skin cancer in Australia. It typically appears as a pale, pearly, or pink spot or lump, sometimes with a translucent or shiny surface. It may look like a small scar or a patch of skin that seems slightly unusual. It rarely causes pain. People often dismiss it as a minor blemish, a cyst, or simply a part of ageing skin. BCCs grow slowly and very rarely spread to other parts of the body, but if left untreated they can cause significant local tissue destruction.
Squamous cell carcinoma (SCC) often appears as a firm pink or red lump, a rough scaly patch, a wart like growth, or an open sore that fails to heal completely. SCCs grow faster than BCCs and carry a greater risk of spreading if not treated. They are commonly found on areas of chronic sun damage including the face, ears, scalp, neck, and backs of the hands.
Neither BCC nor SCC looks like the classic dark melanoma that most people picture. Learning to recognise these less obvious presentations is essential.
Sign 2: A Sore That Does Not Heal
A wound, ulcer, or sore that opens, crusts over, and then reopens without fully healing is one of the most consistently missed warning signs of skin cancer. It is frequently attributed to an insect bite, a minor skin injury, or a reaction to a product, and weeks pass before a doctor is consulted.
Both SCC and BCC can present as a non healing sore. In some cases, the lesion bleeds easily when scratched or rubbed and then appears to be healing, only to open again. Any sore or ulcer on the skin that has not healed within three to four weeks should be assessed by a GP. If you have a lesion that is doing this, our skin cancer clinic at Harbour Town Doctors can assess it promptly with dermoscopic examination.
Sign 3: Changes to an Existing Mole — The ABCDE Guide
The ABCDE criteria were developed to help people and doctors identify suspicious changes in moles and pigmented lesions. Each letter identifies a specific feature that warrants further assessment.
A — Asymmetry
A normal mole, if you drew a line through the centre, should produce two roughly equal halves. An asymmetric mole, where one half does not match the other, is a warning sign. The asymmetry may be subtle and is easy to miss if you are not specifically looking for it.
B — Border
Normal moles have smooth, clearly defined edges. A mole with an irregular, ragged, notched, or blurred border is cause for concern. The edges may appear to fade into the surrounding skin in an uneven way or have a scalloped appearance.
C — Colour
A benign mole is usually a single shade of brown or tan. Multiple colours within a single lesion, including varying shades of brown, black, red, white, or blue, indicate that different cell populations may be present. Uneven colour distribution within the same spot is a significant warning sign.
D — Diameter
Melanomas are often larger than 6 millimetres in diameter when diagnosed, roughly the size of a pencil eraser. However, some melanomas are smaller when detected, and this criterion should not be used in isolation. Any lesion that appears to be growing in size warrants attention regardless of its current measurement.
E — Evolving
This is arguably the most important criterion of all. A lesion that is changing in size, shape, colour, or texture, or that begins to bleed, itch, crust, or feel different, should be seen by a doctor regardless of how it scores against the other criteria. Change is the key signal. Normal moles remain stable over years. An evolving lesion demands prompt assessment.
The ABCDE system is a powerful guide but is not exhaustive. Some melanomas, particularly nodular melanomas, can develop rapidly without following the typical ABCDE pattern. Any new or changing lesion that concerns you should be assessed professionally.
Sign 4: Nodular Melanoma — The Fast Growing Killer
Nodular melanoma is the second most common subtype of melanoma but accounts for a disproportionate number of melanoma deaths because it behaves differently from the standard ABCDE pattern. Rather than spreading outward across the skin surface, nodular melanoma grows downward rapidly. As described by Cancer Council Australia, it typically presents as a raised, dome shaped, firm nodule that may be black, dark brown, blue, or even pink, red, or flesh coloured. It can reach a dangerous thickness within weeks to months.
The danger of nodular melanoma is that it may appear relatively small and recently formed when it is already deep. Because it does not spread laterally across the surface first, it does not develop the irregular borders and colour variations that the ABCDE guide is designed to detect. Many patients describe it as a new lump that appeared quickly and seemed to be enlarging. If you have any rapidly growing raised lesion on your skin, see a doctor urgently.
Sign 5: Lesions on Hidden or Unexpected Areas
Most people check their face, arms, and back. Far fewer check their scalp, the spaces between their toes, the soles of their feet, the palms of their hands, under their fingernails and toenails, the skin of the lower legs, or the areas of the scalp covered by hair. All of these sites are known locations for melanoma development.
Acral lentiginous melanoma is a subtype that specifically affects the palms, soles, and nail beds. It accounts for a small percentage of all melanomas in Australia but is particularly dangerous because it is so frequently discovered late. A dark streak running lengthwise under a fingernail or toenail that is not explained by recent injury should be assessed by a doctor.
Scalp melanomas are also commonly missed because they are concealed by hair. Use a comb to part the hair systematically when doing a self check, or ask a partner to help examine areas you cannot easily see yourself. Your GP will check your scalp during a full skin cancer examination.
Sign 6: A Spot That Looks Like Something Else Entirely
Amelanotic melanoma is a form of melanoma that lacks the dark pigmentation most people associate with the disease. It can appear pink, red, flesh coloured, or only faintly pigmented. Because it looks nothing like a traditional mole or dark lesion, it is frequently mistaken for a pimple, a minor skin infection, a pink scar, or even an inflammatory patch.
Lentigo maligna melanoma is another subtype that is frequently missed. It develops slowly over years within a flat, irregularly shaped, unevenly pigmented patch on sun damaged skin, most commonly the face or neck of older adults. It may resemble an age spot or a sun freckle for a long time before becoming invasive.
The common thread in all missed diagnoses is the assumption that a lesion that looks familiar or benign does not need to be checked. If a spot is new, if it is changing, or if it simply does not look quite right to you, have it seen.
Sign 7: A Spot That Itches, Bleeds, or Feels Different
Skin cancer is not usually painful in its early stages. However, some lesions do itch, particularly BCCs and superficial spreading melanomas. A spot that bleeds with minimal contact, such as when towelling dry or rolling over in bed at night, is a notable warning sign that is easy to attribute to friction or dry skin.
A lesion that crusts and appears to heal slightly before reforming a crust, or one that feels raised, firm, or different in texture from surrounding skin, should be added to the list of lesions to discuss with your doctor at your next visit, or sooner if the change seems rapid.
Who Is at Highest Risk on the Gold Coast?
While anyone can develop skin cancer, certain factors significantly elevate the risk. On the Gold Coast, where UV levels regularly reach extreme ratings and outdoor activity is year round, the following groups should be particularly vigilant.
- People with fair skin, light hair, blue or green eyes, or a tendency to burn rather than tan.
- Those with a personal or family history of melanoma or non melanoma skin cancer.
- People with more than 50 moles, or any atypical or irregular moles.
- Individuals who experienced significant sunburn episodes, particularly in childhood or adolescence.
- Anyone with a history of solarium or tanning bed use.
- Outdoor workers including tradies, farmers, and those in construction or tourism.
- Immunocompromised individuals, including organ transplant recipients.
- People aged over 50, particularly males, in whom melanoma risk and death rates are highest.
How a Professional Skin Check Differs From a Self Examination
A self examination every three months is strongly recommended and can help you identify changes between professional checks. However, it has clear limitations. Most people cannot easily view their entire scalp, back, or the backs of their legs. Self assessment also lacks the magnification and specialised lighting that dermoscopy provides.
A trained doctor using a dermoscope can identify features within a lesion that are completely invisible to the naked eye, including vascular patterns, regression structures, and pigment network irregularities that are strongly associated with malignancy. Professional conduct comprehensive, full body examinations using dermoscopy and provide clear documentation of any lesions identified, along with recommendations for monitoring or biopsy where appropriate.
What to Do If You Find Something Suspicious
Do not wait and watch to see if a suspicious spot gets worse. Do not apply creams or treat it yourself. Do not assume that because it does not hurt it is not serious. See a doctor.
The earlier skin cancer is diagnosed, the simpler and more effective the treatment. Melanoma that is confined to the outermost layer of skin has a five year survival rate approaching 100 percent. Once melanoma spreads to the lymph nodes or distant organs, outcomes become significantly worse. Speed matters.
At Harbour Town Doctors, general practice and family medicine team can address any skin concerns you have, and bulk billing is available for eligible patients.
Conclusion
Skin cancer doesn’t always show obvious warning signs. It can appear as a scar, a pimple, an age spot, or a slow-healing wound. With high UV exposure on the Gold Coast, regular skin checks are essential, not optional. They are one of the smartest and potentially life-saving health decisions you can make each year. contact us today, if you haven’t had a check in the past 12 months or notice any changes.
FAQs: